At the same time, local educators training the next generation of nurses said programming was temporarily paused; already-limited capacities in clinical programs became even more restrictive; and graduations were delayed.
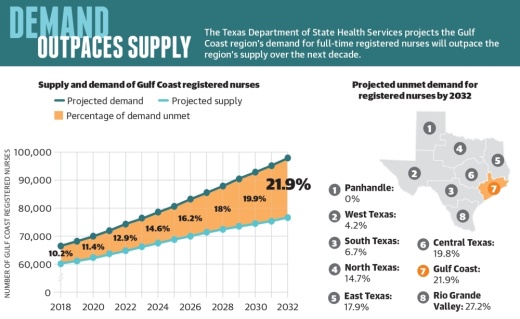
But hospitals across the state have faced nursing shortages since long before the pandemic, health care officials said. The Texas Department of State Health Services projects the Gulf Coast region will have a deficit of 21,400 registered nurses by 2032 as the growing demand continues to outweigh the supply.
“Health care workforce shortages existed before the pandemic. We didn’t have enough doctors; we didn’t have enough nurses, and the pandemic has definitely exacerbated that problem,” American Medical Association President Susan Bailey said.
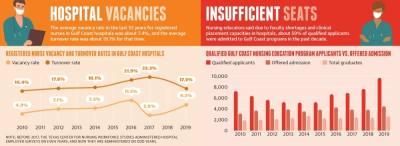
The median turnover rate for registered nurses in Gulf Coast hospitals was 17.5% in 2019, according to DSHS data. Since the pandemic began, many nurses have considered leaving the profession between the anxiety over bringing COVID-19 home to their families and losing at least 4,000 health care workers to the virus nationally, Bailey said.
In the last decade, the Gulf Coast region’s supply of registered nurses has grown by 45%, per the DSHS, but that growth is not enough to keep up with the population. Nursing education leaders said there is not a shortage of individuals interested in the profession, but training programs are competitive and expensive.
Nickie Loftin, nursing program director at Lone Star College-Kingwood, said 1,500 individuals applied to the college’s nursing program in January, but the college can only accept 100 applicants to its registered nursing program, 60 for its transition program and 24 for the licensed vocational nursing program each year.
While the college used to accept 80 students per year to its RN program, it increased its capacity to 100 students this spring semester, she said.
“I’m trying to increase my enrollment as much as I possibly can to meet the demands of the community, but at the same time having to balance the ability to educate those extra students,” Loftin said. “It’s a tightrope walk that I do to try to meet everybody’s demands.”
Shortage factors
While the pandemic amplified the state’s nursing shortage, experts said it has been a concern for many years.
“As our nursing workforce is aging and our population is aging, the nurses are retiring at a greater rate than we can hire, and our patient volume is increasing,” said Kelli Nations, chief nursing executive for HCA Houston Healthcare, which has a hospital in Kingwood.
About 24% of the region’s registered nursing workforce in 2019 was older than 55, per the DSHS.
COVID-19 has also led to more nurses retiring early than hospitals would see in a typical year, said Dr. Renae Schumann, the former dean of Houston Baptist University’s School of Nursing and Allied Health who now serves as District 9 president of the Texas Nurses Association.
Additionally, others transitioned to travel nursing to serve other COVID-19 hot spots, said John Corbeil, CEO of HCA Houston Healthcare Kingwood. He said the nursing shortage is the biggest operational challenge the hospital is facing as the hospital ramps up recruitment to backfill the vacant positions.
“Hopefully as things start to calm down with COVID nationwide, those nursing colleagues will move back home to Houston, and we’ll be able to backfill those open vacancies,” he said.
HCA Houston Healthcare also donated $3.5 million in April 2019 to the University of Houston College of Nursing to help the college add more adjunct and full-time faculty members at HCA’s affiliated facilities as well as support the simulation center at the college’s future Katy campus, hospital officials said.
The hospital also acquired the Galen College of Nursing last year to create a pathway from training nurses to offering them employment in the hospital system, Corbeil said.
Education programs
As the demand for nurses increases, numerous programs in the Lake Houston area are training future nurses. Humble and New Caney ISDs both offer nursing programs through their respective career and technical education programs.
In HISD, students who complete the district’s nursing CTE program can earn an associate degree while becoming a certified nursing assistant, or a CNA. Shirley Revels, a registered nurse who teaches nursing at HISD, said most students graduate with jobs at long-term care facilities.
“Students realize that when they go into a health science field, they have a guaranteed job,” she said. “They know they’re going to have a job when they finish. Even when they get out of high school, most of my students are already employed as CNAs.”
Amid the pandemic, the district’s 40 CNA students were required to attend in-person classes rather than virtual to get hands-on experience, Revels said. However, students were not allowed to visit• long-term care facilities for their 40 hours of clinical experience due to the risk of COVID-19 exposure, she said.
Brooke Lyles, NCISD’s CTE director of education, said the district offers four-year health science clusters at Porter and New Caney high schools. The district partners with the Montgomery County Hospital District to certify students to become CNAs, emergency medical technicians or phlebotomists.
Despite these offerings, faculty shortages and clinical placement capacities limit the number of new nurses produced every year. The DSHS reported 54% of qualified applicants were not granted admission to one of the region’s 27 prelicensure registered nurse education programs in 2019 due to a limited number of seats available.
The Texas Legislature created the Nursing Shortage Reduction Program in 2001, allowing the Texas Higher Education Coordinating Board to provide dedicated funds to nursing education programs that increase the number of nursing graduates. According to the Texas Nurses Association, the number of new nurses produced grew by nearly 180% from 2002-19.
Expanding offerings
To meet the growing demand for HISD’s nursing program, the district is building its new health science wing at Kingwood High School, Revels said.
When it opens in August 2022, the wing will feature more lab space and an intensive care unit. HISD officials said via email the new health science wing could expand the on-campus program capacity of heath science courses once built.
Meanwhile, LSC-Kingwood will finish building its $18.8 million Lone Star Health Professions Center this fall, which is funded by LSC’s 2014 bond and will be the new home of nursing and four other health-related industries starting in spring 2022.
While nursing classes are currently being held at the campus’s Science Instructional Building, Loftin said the new facility will double the program’s hospital beds and feature a state-of-the-art simulation lab, two intensive care units, a labor and delivery suite, a home health room and eight medical service beds.
This new space will allow Loftin to slowly increase nursing program admissions at the college, she said. In its first few years, Loftin said she hopes to increase admissions by 10% for each group each year.
However, finding faculty to teach students is another challenge altogether, she said. Hospitals are only able to accept a few students for clinical placements, and the college can only have 10 students per faculty member, she said.
“While you might not make as much money [as a faculty member], you will have more time off, and you’ll have weekends off and holidays off,” she said. “It’s just a matter of making your trades in life and loving what you do.”