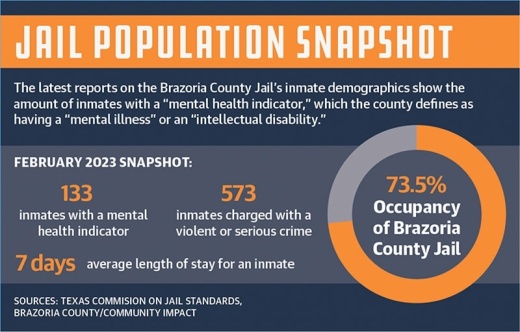
The county is in the process of negotiating a contract with Inspired Behavioral Health Inc., a third-party firm that may assist the Brazoria County Jail in treating nonviolent inmates in need of mental health care, Brazoria County Judge Matt Sebesta said.
“We’re holding a lot of patients, inmates, that need to be in a mental health facility and receiving the things that they need to receive to get them healthy and get them out of jail,” Sebesta said.
Sebesta previously said the Inspired Behavioral Health facility would be able to take in up to 16 incarcerated people at a time. A possible contract is tentatively on hold as the company undergoes reorganization, according to County Public Information Officer Sharon Trower.
The county’s move toward outside support comes as Texas is facing an unprecedented staffing shortage across state-run hospitals. A Texas Health and Human Services Commission news release from Jan. 24 states more than 700 state hospital beds are unstaffed “due to workforce challenges.”
Sebesta said these staffing shortages are slowing the transfer of inmates needing state hospital care out of the county jail system, which the Texas Association of Counties referred to as the largest mental health system in the state in a December 2020 legislative issue brief.
“The largest mental health facilities in the state of Texas are county jails. That is where most of the folks that have mental health issues are being housed,” Sebesta said.
State bed shortage
The HHSC announced Jan. 24 it is increasing salaries and starting pay at state hospitals to help with “crucial staffing needs” and bring back some of the 700 unstaffed beds.
In the release, HHSC stated it is looking to fill about 1,805 vacancies in state hospitals and 2,137 across the 13 state-supported living centers, which HHSC says provide “campus-based direct services and support to people with intellectual and developmental disabilities.”
Krishnaveni Gundu, executive director of the Texas Jail Project, a nonprofit organization that advocates for jail reform, said a large portion of occupied state hospital beds are essentially “stuck.” She said up to 50% of occupied beds are being used by individuals who need long-term care, and due to having acute needs, there is nowhere for them to be transferred out.
“There’s nowhere for these people to go,” Gundu said. “So if we don’t have a plan to get that population out, it doesn’t matter how many beds we build.”
A slowdown in state support due to the staffing issues is compounded by a gradual increase in the inmate population at the jail. Sebesta said the county jail faced crowding issues in August-September 2022, when it reached up to 1,000 inmates—nearly 90% of the jail’s capacity.
Brandon Wood, director of the Texas Commission on Jail Standards, previously told Community Impact that counties aim to keep their jails under 90% of their capacity because jail beds have certain classifications that make jail operations difficult above that level. Wood said he was looking to see legislation this session that would help address jail populations.
“There’s always the potential for legislation that deals with criminal justice to have an impact on our jail populations,” Wood said. “It can range from increase[s] in penalt[ies], looking at the dollar amounts associated with the type of charges that can be filed [or] whether there’s any movement on the mental health side.”
The cost on counties
The buildup of inmates and state staffing issues force the county to foot the bill for people awaiting transfer.
Sebesta said holding inmates for the state costs the county a significant amount. He called for the state to reimburse counties for holding inmates that are ready to be transferred into state systems, where inmates can receive specialized care that counties may not be able to provide.
“We end up holding a lot of their inmates for too long. ... When they don’t take them in a timely manner, we’re still hanging on to them, and folks are being double taxed because we’re having to pay local tax dollars to house those inmates when they should be in the state system,” Sebesta said.
Sebesta said it costs counties about $51 a day per person to house people that await transfer to a state facility. He said their transfer allows for state and federal programs to help cover their needs without use of local tax dollars to fund holding people at the jail, which he said adds up quickly.
“There are some programs that [the state] can utilize with them that are not available to us when they’re in our care,” Sebesta said. “When they are in our care, they are completely on the taxpayers’ dime for all their medications [and] health care needs.”
The bigger picture
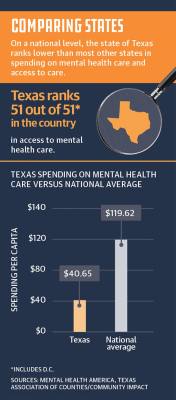
In both 2022 and 2023, Texas was ranked the lowest state in the country in access to mental health care, according to annual reports from Mental Health America released those years.
Multiple house bills have been filed during the 88th legislative session regarding mental health in state facilities and jails. House Joint Resolution 90 filed Jan. 26 by Rep. Elizabeth Campos, D-San Antonio, proposed the use of general obligation bonds to fund the construction, expansion and maintenance of state mental health facilities.
Meanwhile, state Rep. David Spiller, R-Jacksboro, filed HB 2233 on Feb. 13 to require mental health awareness training for first responders.
“This has been an issue that’s probably been going on for decades; the state has never adequately funded mental health resources,” Sebesta said. “It’s not a sexy topic; it’s an expensive topic, so it’s not going to get as much attention in Austin as it needs to get.”
Rachel Carlton contributed to this report